Spinal Issues and Axial Spondyloarthritis
Reviewed by: HU Medical Review Board | Last reviewed: January 2023 | Last updated: August 2024
Axial spondyloarthritis (axSpA) is a type of arthritis that can cause inflammation in both the joints and the places where tendons and ligaments attach to the joints (entheses). AxSpA almost always affects the spine, but it can cause pain in other places too.1
What spinal issues can occur with axial spondyloarthritis?
As axSpA progresses, chronic inflammation can wear away at the bone of the joints. The body then works to replace the bone that was lost. As a result, it may make too much bone. This can eventually cause the joint to fuse or join together. Called spinal fusion, this outcome may occur in people with ankylosing spondylitis (AS).1-3
The joints, tendons, and ligaments of the spine also can become calcified and hard. This makes the spine harder to move and less flexible. On an X-ray image, the spine may look like bamboo, so it is sometimes called “bamboo spine.”1-3
Spinal fusion and bamboo spine can lead to other problems with the spine, including spinal fractures, kyphosis, and stenosis.1
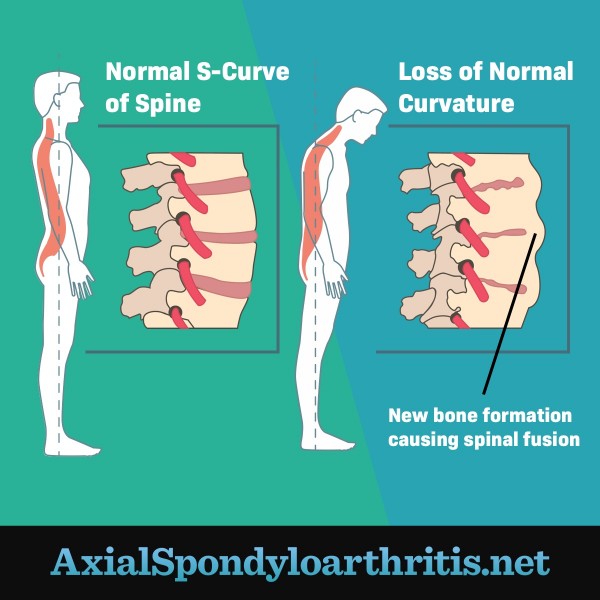
Figure 1. A normal spine versus a fused spine due to progressed AxSpA
Spinal fractures
Spinal fractures are cracks or breaks in the bones of the spine (vertebrae). These fractures may occur in the lower back (lumbar spine), middle back (thoracic spine), or neck (cervical spine). The fractures can range from mild to severe.4
When AS begins to cause spinal fusion, your spine cannot move as much. This makes it less stable. The fused joints are weak and brittle, and they put you at increased risk of spinal fractures. A spinal fracture can happen from an accident, like a car crash, or from doing a common task, like reaching for something.1,4
Osteoporosis is another condition that can weaken bones and increase the risk of spinal fractures. People with axSpA are at an increased risk of osteoporosis. They are much more likely to have spinal fractures than people who do not have axSpA.1,5,6
A mild spinal fracture might not hurt, and you may not know it happened. But a severe spinal fracture can cause a lot of pain and damage your spinal cord. Fractures in the lower or middle back can cause pain that is worse with movement. Neck fractures are the most dangerous, because they increase the risk of neurologic damage and can even lead to death.4,5
Treatment for spinal fractures may involve physical therapy, a brace, or surgery.4,5
Kyphosis
Kyphosis is an outward curvature of the spine, which can cause a hunched or rounded back. This can lead to a forward-stooped posture. In some cases, kyphosis can affect your ability to inflate your lungs fully. Kyphosis can vary from mild to severe. More severe curvatures tend to cause more pain.1,7
With advances in treating axSpA, kyphosis is now less common, although it can occur in severe cases. Severe kyphosis may require surgery to reduce pain and deformity and increase your quality of life.8
Stenosis
Spinal stenosis is a narrowing of the spinal column, where the spinal cord is located. It may affect the spaces where nerves branch out from the spinal cord to the rest of the body or the spaces between vertebrae.9,10
Spinal stenosis can cause pain in the back or arms and legs. It may also cause numbness or weakness in the arms or legs. A severe type of spinal stenosis called cauda equina syndrome can lead to a loss of bowel or bladder control. Treatment for spinal stenosis may involve medicines to reduce the pain or surgery to correct nerve damage.9